
Medicare Special Needs Plan sign-ups exceeded expectations from CMS during the 2025 annual enrollment period, offering a welcome boost to an otherwise slowing Medicare Advantage market.
These products are a key to growth for Medicare Advantage, even though the rate of increase slowed from 13% in 2024 to 10% in 2025.
By comparison, enrollment in standard Medicare Advantage plans rose at one of the slowest paces in program history this year, amid heightened scrutiny from regulators and lawmakers.
More than 7.3 million people were enrolled in Special Needs Plans as of Feb. 1, up 10.1% from a year before. Enrollment in SNPs accounts for 20% of Medicare Advantage enrollment in 2024, an increase from 12% in 2010.
D-SNPs Lead the Way for Growth
Insurers invested in SNPs, adding generous supplemental benefits and entering new geographic markets. Medicare Advantage insurers report generating the highest profit margins from D-SNPs.
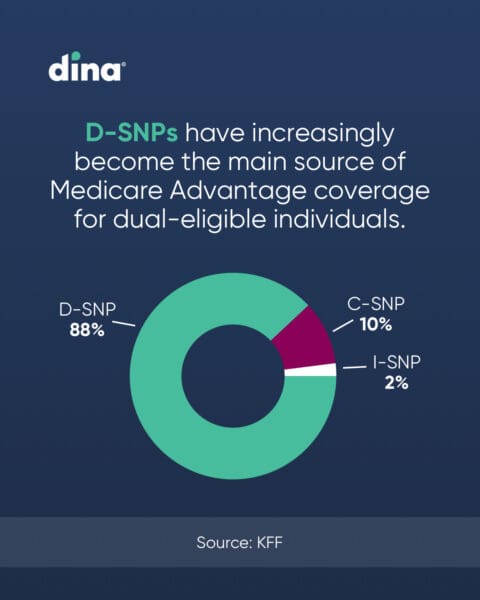
D-SNPs have increasingly become the main source of Medicare Advantage coverage for dual-eligible individuals and account for 88% of SNP enrollments.
D-SNPs are required to provide greater coordination of Medicare and Medicaid benefits than other Medicare Advantage plans to improve coordination across programs and patient outcomes.
D-SNPs typically provide benefits not otherwise available in traditional Medicare and generally do not charge a premium.
“There is a growing need to make available a suite of both medical and non-medical benefits–and promote utilization–as there is evidence that it will reduce total costs and improve quality and the member experience,” said Travis Woyner, Dina’s SVP of strategy.
“The challenge SNP plans now have is implementing a mechanism to collect and analyze data so they can measure the impact of these services.”
D-SNP Enrollment Varies by State
SNP enrollment has more than doubled since 2019, due in part to the increasing number of SNP plans available on average and more dual eligible individuals with access to these plans.
About 12.9 million people received health coverage under both Medicare and Medicaid in 2021. Dual-eligible individuals are a diverse group, as nearly half are people of color and nearly 40% are under age 65. However, this group of people share some common characteristics, such as limited financial means and health care needs that are more wide-ranging and complex than the average Medicare enrollee.
The challenge is implementing a mechanism to collect and analyze data so SNPs can measure the impact of these services.
In 2021, D-SNP enrollment as a share of dual-eligible individuals ranged from 5% in Nevada to 58% in Hawaii, as compared to 29% nationwide. In seven states, 40% or more of all dual-eligible individuals were enrolled in D-SNPs: Alabama (42%), New York (42%), Florida (46%), Tennessee (46%), Arizona (47%), and Hawaii (58%), as well as in Puerto Rico (98%). Conversely, less than 10% of dual-eligible individuals were enrolled in D-SNPs in Nevada (5%) and Montana (8%).
New D-SNP Enrollment Periods
Beginning January 1, 2025, enrollment changes include a new integrated care Special Enrollment Period (SEP) that allows monthly enrollment in select D-SNP plans and Medicaid plans under one insurer. This new SEP is available to people who are eligible for Medicare and have full Medicaid benefits and replaces the previous quarterly SEP.
All dual-eligible beneficiaries can still enroll during the Annual Enrollment Period (AEP) and the Medicare Special Enrollment Period with a qualifying life event.
While enrollment and plan availability continue to grow, it is not clear how well D-SNPs coordinate with Medicaid to provide the full range of benefits to dual-eligible enrollees. Fewer than one in ten D-SNP enrollees are in fully integrated plans.
These changes are designed to facilitate aligned enrollment and enhance care coordination and benefit options for members.

Rising Medical Expenses?
Don't Cut Benefits!
Instead, see how to drive smart utilization of non-medical benefits to meet your value-based objectives. Download the report "Rising Medical Expenses? How to Use Supplemental Benefits to Manage Total Cost of Care" to learn more.





